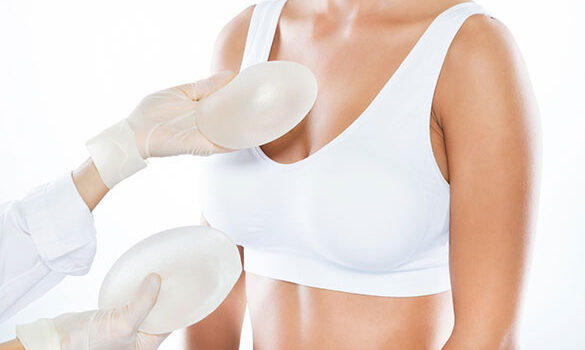
Restoring Wholeness and Confidence
Breast reconstruction offers a new beginning for those affected by breast cancer or other conditions leading to mastectomy or breast removal. This procedure aims to rebuild the breast to near its normal shape, appearance, and size, restoring a sense of wholeness and confidence. Utilizing advanced surgical techniques, we can create a breast that closely matches your natural breast in form and appearance.
Procedure Type
Body Surgery
Anesthesia
General
Procedure Duration
2-6 hours
Pain Level
5/10
Recovery Time
4-6 weeks
Resumption of Physical Activities
6-8 weeks
Ideal for Treating
Breast Reconstruction Benefits
Find a Clinic for this procedure- Restores a natural-looking breast shape after mastectomy.
- Rebuilds confidence and self-esteem.
- Offers closure and a sense of normalcy post-cancer treatment.
- Enables clothes to fit better.
- Can be performed immediately following mastectomy or delayed until after other treatments.
The GraceMed difference
Our plastic and cosmetic surgeons, dermatologists, and medical spa experts are dedicated to providing exceptional service and top quality care to all our patients. No procedure is ever rushed. No detail skipped. No compromise accepted. We don’t accept anything less. And neither should you.
Personalized solutions
Expect a custom treatment plan based on your desired goals.
State-of-the-art technology
Clinically-proven treatments backed by the latest technology and equipment.
Experienced medical leaders
Our expert medical staff ensure you always get the very best care.

Procedure and Recovery
Breast reconstruction can be achieved through various methods, including implant-based reconstruction or using your own tissue (flap reconstruction). The choice depends on individual cases, medical history, and personal preferences. The process might involve several stages for optimal results.
Recovery varies based on the reconstruction method. Initial discomfort, swelling, and bruising are common but manageable with medication. Follow-up visits are necessary for monitoring progress and addressing any concerns.
Risks include infection, bleeding, and issues related to implant or flap procedures. Long-term, there might be the need for revision surgeries or adjustments.
GraceMed Breast Reconstruction Specialists
Breast Reconstruction Clinics
The following GraceMed clinics perform breast reconstruction procedures. Contact your local clinic for a consultation and find out about promotions or packages that might be available to you.
FAQs
Affordable Monthly Payments
At GraceMed, we understand that financing cosmetic procedures is a significant personal investment. That’s why we’ve partnered with Beautifi, a Canadian company that offers industry-leading interest rates and affordable monthly payment options for cosmetic procedures.